A Miracle Pregnancy
After giving birth to Jackson, our first child, I faced a silent struggle that many women know too well. My body wouldn’t ovulate, and month after month brought more disappointment. Eventually, with the help of a fertility specialist, our prayers were answered – I was pregnant! Audrey was our miracle baby, a longed-for gift we had hoped for with all our hearts.
As thrilled as I was to be pregnant again, the memories of my first birth still haunted me. My first birth had been traumatic. During labour with Jackson, I developed severe preeclampsia—so sudden and life-threatening that I ended up in ICU for several days, while Jackson spent 10 long days in the Special Care Nursery. The trauma lingered, and with my second pregnancy, I was monitored very closely.
During our 20-week scan, my fears became a reality. The doctors told me I had Vasa Previa—a rare and life-threatening condition where the baby’s blood vessels lay across the cervix. If labour started naturally, those fragile blood vessels would rupture, and Audrey could be gone in minutes. I was told I’d need a planned caesarean to ensure Audrey’s safe arrival. I can still remember the wave of fear washing over me, even as I smiled and nodded, trying to absorb their words.
From that moment on, I knew it was time to slow down and take extra special care of myself.
The Day My Waters Broke
At 26 weeks, while working in the Executive Unit of a local hospital, I felt a strange leaking sensation. Filled with panic I slowly made my way to the bathroom praying that there wasn’t any blood from the Vasa Previa. I was relieved to see that it was only clear liquid, and I didn’t think too much of it at first. I went back to my desk and continued to work until about 20 minutes later when the liquid started running down my legs. At this point the panic started to set in, and I urgently called my Obstetrician. I was advised to make my way to the Private Hospital where he would meet me to investigate what was happening. My mother-in-law drove me straight to the hospital where my Obstetrician tested the leaking fluid and discovered that it was amniotic fluid and this meant that my waters had broken.
To be honest, in this moment my head was spinning. I couldn’t believe that my waters had broken and didn’t really understand what this meant as I had never known anyone to have a premature baby and had no idea what journey laid ahead. I was sent straight to the Royal Hospital for Women by ambulance where we would be able to access the Neonatal Intensive Care Unit (NICU) and the outstanding pre-natal care.
As soon as I arrived, I was greeted by the amazing nursing staff and they tried to put my mind at ease whilst still being honest about my situation. I was given my first steroid injection to help the baby’s lungs develop in preparation for a premature delivery and help give her a fighting chance at survival.
Three Weeks of Waiting
I was placed on strict bed rest. Those three weeks of bed rest felt endless. I was confined to a hospital bed, separated from my husband and my little boy, and the loneliness often brought me to tears. All I wanted was to tuck Jackson in at night and feel the comfort of being at home. My heart was constantly torn in two. But I clung to one thing: knowing that every single day Audrey stayed inside me meant four fewer days she would spend in the NICU. Holding onto that truth gave me the strength I needed to keep going
My belly shrank week by week as amniotic fluid leaked away. It’s such a surreal and heartbreaking feeling. Most mothers marvel as their bellies grow rounder, fuller, proof that their baby is thriving. Each night I would rub my shrinking belly and whisper to Audrey, “Hold on, little one. We can do this.” Watching myself grow smaller while my fear grew bigger was a feeling I will never forget.
On top of everything else, our family history of Hereditary Fructose Intolerance (HFI) weighed heavily on my mind. Audrey had a 1 in 4 chance of inheriting it, and I couldn’t take any risks. From the very beginning, I made sure every doctor and nurse knew she had to be treated as though she already had HFI. I sat down with specialists and even the head of department to explain what this meant. The thought that one wrong medication or supplement could harm her was terrifying. So, preparing the staff that would be looking after her was my way of protecting her, especially when so much felt out of my hands.
Christmas Day — and Labour Begins
It was Christmas Day, a day that should have been filled with nothing but joy. My family joined me at the hospital for a special Christmas lunch, and I soaked up every precious moment, listening to Jackson’s excitement as he shared all about the presents Santa had brought him. My heart was so full of love, even though my body was so very tired. That night, I drifted off to sleep feeling happy, grateful, and content.
But at midnight, everything changed. I woke to find I was bleeding. In that terrifying moment, we didn’t know if it was my blood or our baby’s. A nurse was assigned to sit at my bedside all night, her quiet presence both comforting and terrifying. Contractions began—low, strong, unmistakable—even though they weren’t registering on the monitors. They grew closer, harder, relentless.
By 7am, I was rushed to theatre. The Registrars frantically contacted the specialist, trying to determine the safest path forward. My contractions were now relentless, and I could feel my body preparing for labour. My fear grew—I knew the risk of Vasa Previa was far too great. Within moments, everything spiralled into urgency, and I was wheeled into theatre for an emergency caesarean.
My husband didn’t make it in time to be by my side, but he arrived just in time to meet our beautiful little girl. At 7:00am on 26 December, Audrey was born at just 29 weeks.
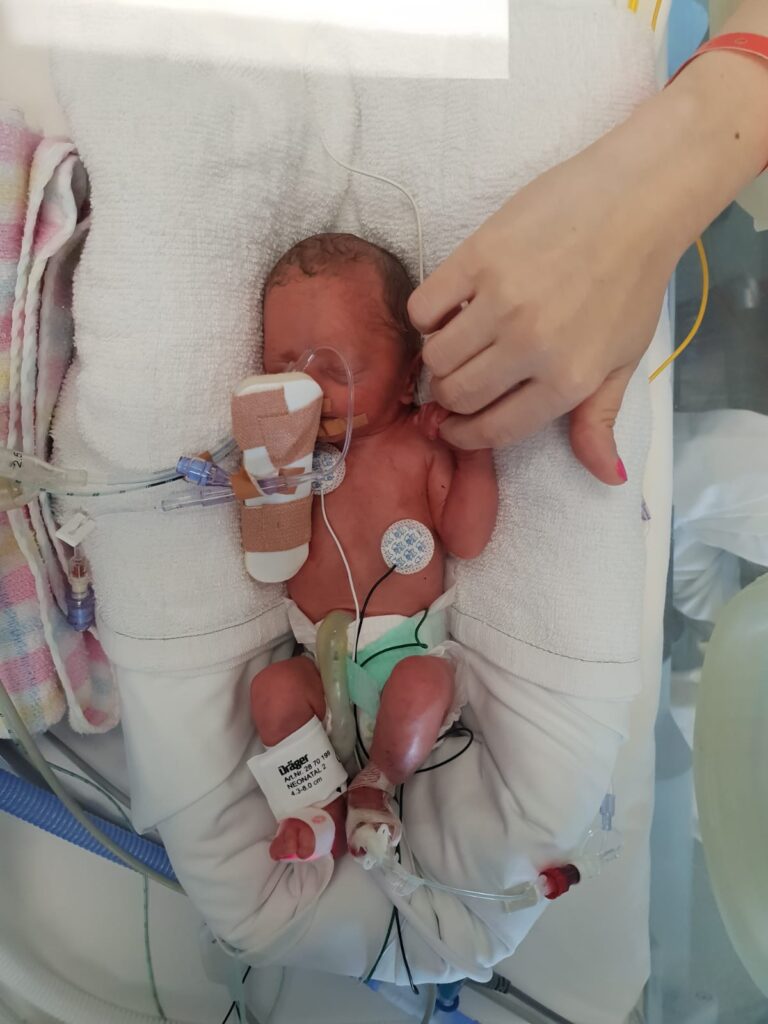
Our tiny Christmas miracle, our premmie warrior, entered this world weighing just 1000 grams—so fragile, yet already showing the strength that would come to define her journey.
As soon as Audrey was delivered, there was no joyous moment of her being held up high for me to see. Her tiny, delicate lungs were far too fragile for that. Instead, the Anesthetist gently propped me up so that I could catch my very first glimpse of my baby girl. She was perfect. Tiny—so impossibly tiny—but perfect. The rush of relief that swept over me was overwhelming. She was here. She was alive. She was safe. In that moment, I felt like we had survived the very first of many obstacles together.
NICU: A New Kind of Motherhood
Within minutes, Audrey was whisked away to the NICU. Ashley followed closely behind as I was taken to recovery, desperate for news. Hours later, in a wheelchair, I finally made my way to see her. Seeing her precious little face, knowing she was stable, was the greatest comfort. She was hooked up to a CPAP machine, which would help her breathe for the next four weeks. The wires, machines, and constant beeping were confronting, but when I looked past them, I saw only my beautiful daughter fighting so bravely.
It wasn’t until three days later that I got to hold Audrey for the very first time. Skin-to-skin, heart to heart. That moment is forever etched in my soul—it gave me strength, it gave me hope, and it reminded me that no matter how hard this journey was, we were in it together.
I stayed in hospital for one week before being discharged home. The thought of leaving my little girl behind broke me. I was discharged on New Year’s Eve and it was one of the hardest nights of my life. I came home empty-handed, my arms aching for my baby, my heart split between two children who both needed me. I cried most of the night, but the NICU nurses were angels, assuring me that I could call anytime, day or night, to check in on Audrey. Their kindness was a lifeline.
The weeks that followed were filled with expressing milk every three hours, around the clock, without my baby there to feed. It was exhausting, but it was my way of nurturing her, of doing something tangible to help her grow stronger. Ashley drove me to the hospital every single day, his love and support meant everything. We would deliver milk, take part in her daily “cares,” and then—my most cherished moment—have our one-hour cuddle. Only one cuddle a day was allowed, because rest was vital for her growth. That one precious hour was everything to me. I held onto it, treasured it, and counted down the hours until the next.
At two weeks old, Audrey became anaemic. She needed iron, but every supplement available contained fructose and wasn’t safe for her. The only option was a blood transfusion. The thought of her tiny body enduring something so serious broke me, but once again, she proved herself a warrior. She handled it with such strength, reminding me she was braver than I ever imagined.
By four weeks, through genetic testing we received confirmation of what we had already suspected—Audrey had Hereditary Fructose Intolerance, just like her brother. It was a heavy truth to face, but we also knew it was manageable, and she was in the best possible care. Step by step, she progressed—moving from CPAP to high-flow oxygen, and then to low-flow oxygen. Each milestone felt monumental, each step forward a victory worth celebrating.
Special Care Nursery
At six weeks, Audrey graduated to the Special Care Nursery. Soon after, she was transferred to a private hospital just five minutes from home. Having her so close was a gift. I could visit multiple times a day, be there for her feeds, bath times, and endless cuddles. Slowly, we learned to breastfeed together. Every small success felt like a miracle. At ten weeks old, she was strong enough to have her feeding tube removed. For the very first time, I saw her beautiful face without a single piece of medical equipment. I will never forget that moment—she quite literally took my breath away.
Finally, at ten weeks (39 weeks and 4 days gestation), Audrey weighed 3080 grams. She was discharged home, and we were finally complete as a family of four. I was nervous—she still felt so tiny, so fragile—but more than anything, I was overwhelmed with joy. After everything, she was home, in my arms, whenever I wanted, without limits or timeframes.
The journey was long and at times heartbreaking, but also filled with awe, gratitude, and love. I wish I had known more about premature babies before living this experience. It’s so much more common than I ever realised, and I now understand deeply just how extraordinary the care, equipment, and dedication of NICU teams truly are. Much of the lifesaving equipment that gave Audrey her chance at life is funded by community charities, and I will be forever thankful for their work.
Our little Christmas miracle fought every step of the way to be here. Audrey’s journey into the world wasn’t what we had imagined—but it shaped her into the resilient, determined little girl she is today. And it shaped us too—reminding us every day never to take a single moment for granted.
Audrey’s HFI Newborn Journey
Audrey’s early months at home brought a new layer of challenges. With her confirmed diagnosis of Hereditary Fructose Intolerance, every choice we made about feeding and nutrition carried weight. We couldn’t rely on standard newborn formulas or baby foods, as so many contained hidden fructose, sucrose, or unsafe additives. Together with our specialist team, we worked tirelessly to find a safe formula option that would support her fragile start in life without compromising her health.
When Audrey developed iron deficiency as a newborn, the challenge became even greater. All the iron supplements available at the time contained fructose and were unsafe for her. I remember feeling overwhelmed, but determined. I immediately started researching potential recipes that may be able to help her and created a special liver purée recipe to give her the iron she so desperately needed.
As Audrey grew, the challenges continued. Homemade purees became part of our routine, crafted with absolute care to ensure they were completely fructose free. Even simple milestones like teething brought their own hurdles, as we had to create safe, homemade rusks she could gnaw on without risk. Each stage required extra planning, creativity, and vigilance—but also gave us a sense of empowerment. We weren’t just nourishing her body—we were protecting her future.
This journey has shown me that while HFI adds challenges to early motherhood, it also brings an even deeper connection. Every safe feed, every small adaptation, every milestone was a reminder that Audrey could not only survive, but truly thrive. She is living proof that love, persistence, and careful planning can overcome even the toughest obstacles.